The healthiest city in the world - Prof Andrew Corbett-Nolan
13 May 2022
Our chief executive Professor Andrew Corbett-Nolan explores what it will take for London to realise its vision of becoming the healthiest global city and what all places can do to be healthier.
The NHS in London and the Mayor have a joint vision for London to become the world’s healthiest city. It may seem an implausible ambition especially for the capital city of a country with a rising obesity crisis, food poverty, a fuel and climate crisis, vulnerable to the negative impacts of Brexit, especially around supply. But as a dear colleague of mine often says: “Rome may not have been built in a day, but it did get built.”
At a recent GGI breakfast seminar I chaired, we discussed how to initiate this work, outlining the key building blocks: partnerships and integration, anchor institutions and healthcare.
An expanding remit for the NHS
Under new Integrated Care Systems (ICSs), NHS organisations will have broader roles and responsibilities for health and wellbeing, expanding into the sphere of social and economic development. The four key aims of ICSs are:
- improve outcomes in population health and healthcare
- tackle inequalities in outcomes, experience, and access
- enhance productivity and value for money
- help the NHS support broader social and economic development.
NHS priorities branching out from COVID to addressing the backlog, system working and contributing to population health management, and their closer collaborative and integrated work with local authorities, VCSE organisations and other public bodies, will be critical to London achieving its vision and for any place aiming to be healthier.
Partnerships and integration
Partnerships in London are tangibly delivering. Managing the pandemic would not have been possible without boroughs and the NHS working together and longer term the Mayor has committed to health being part of all city policies. This has led to the huge improvements to air quality. The London Estates Development Unit (LEDU) is leading the way to unlocking some of the NHS estate to create decent houses. Clean air and decent homes are two important determinants of good health.
The NHS enjoys huge trust from the public. For example, work from Imperial College Health Partners finding that 98% expressed an expectation that all health and care organisations in London join-up de-personalised information, as part of a population dataset, to support proactive care, planning, and research and development. Can the NHS leverage this to support broader trust in health living messaging, and could sharing data between public sector bodies help to identify individuals who need early intervention?
Anchor Institutions
The NHS budget is equivalent to the GDP of Greece, and London’s share of this is £24bn. The NHS in London employs a quarter of a million people, and over the last three years the WTE headcount has increased by 15.6%. Whilst NHS jobs are good ones with decent pension provision NHS organisations have not committed to the living wage, which in London is £11.05 an hour. Agenda for Change band 2s in outer London will be earning less than this, and though the Skills Academy is supporting people into entry level jobs there is an uneven playing field between the NHS and social care.
Anchor institutions should think of joining the Living Wage Foundation (GGI has been a member for a decade) and using procurement as a means of putting people into work locally. London will be the first region to launch the social value toolkit to guide procurement.
Healthcare
The challenges for health services themselves are significant, with now one million Londoners on waiting lists and the concomitant effect on their lives and those of their families too. Alongside better system working immunisation and changes to out of hospital care will form very much a feature of the coming year.
Vaccination is the most cost effective of all health interventions. The pandemic has transformed vaccination rates, and some of the innovations to drive up COVID vaccination rates can be mainstreamed.
The shortly to be published Fuller Report (GGI have worked with Dr Claire Fuller over several years supporting the development of Surrey Heartlands ICS) will talk to the creation of a new national model for primary care teams, perhaps involving integrated, multi-disciplinary teams as the standard.
Finally, has the time come for the NHS to start to enter the social care market? In many ways this could have benefits, for example by providing entry level jobs as well as ensuring social care provision where not viable or sustainable for private operators.
Learning and improving
Critical to this work will be how the NHS, local authorities, VCSE organisations and other organisations at the heart of driving health and wellbeing improvement at place through new ICSs, create learning systems. To realise ambitious targets, these organisations will need to innovate, take risks and try new methods and approaches to longstanding challenges. Feedback and data driven decision making will be key.
Feedback loops, also known as causal loop diagrams, are a tool to help visualise these cause and effect relationships within a system. Feedback loops can be positive or negative, reinforcing or counteracting/balancing. The loops show the relationship of the parts in the system and model the impact on the system of possible interventions, including the unintended consequences.
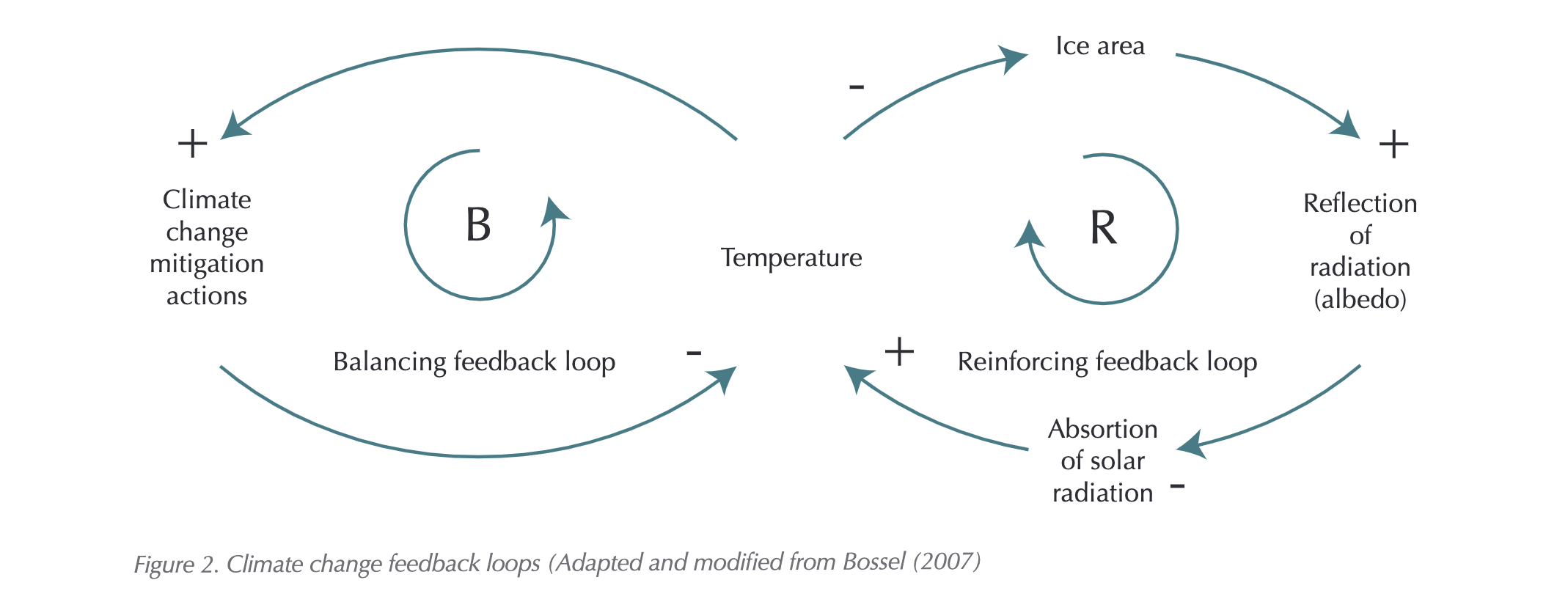
It takes time to achieve real change, especially that which is ambitious. It takes a process of continued development and improvement to achieve impactful outcomes. However, the discussion that took place demonstrated to me that there is both a real appetite amongst our health and social care colleagues to get this right for the patients and citizens that they serve, as well as a bevy of innovative actions and ideas that can be developed and implemented.
